Dr. Ronine Zamor gives us a great overview of the of neonatal shock, and highlights the times when those babies don’t follow “the rules.”
Differential Diagnosis of Neonatal Shock
The differential diagnosis of neonatal shock are within the same 4 categories as in adults. However, there is one critical difference in neonates, and it surrounds the heart! It is important to keep in mind how specific ductal dependent lesions can present as the PDA closes, and how that can contribute to neonatal shock.
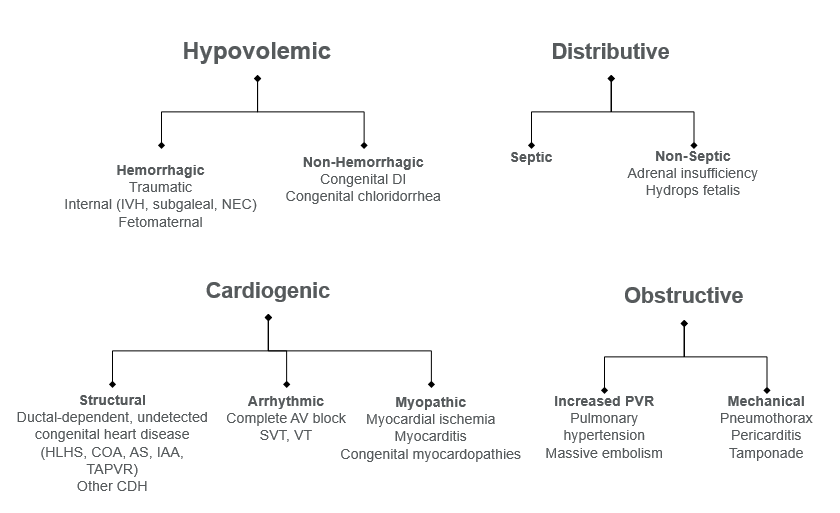
Remember to evaluate with Chest X-ray and stat ECHO if you are worried about the heart. Give prostaglandins! Side effects of prostaglandins include apnea, vasodilation, bradycardia. But in a critically ill neonate, you may have these findings anyway…
Those really, really tiny vessels...
Everyone knows these babies are some of the hardest to obtain vascular access on. Some pointers to keep in mind:
Umbilical Lines
Umbilical lines are best done under sterile conditions. However, this is not as familiar among emergency medicine providers and can take a very long time to obtain.
The NEJM has a great video that reviews the procedure here. [1]
Intraosseous Access
Intraosseous Access is more familiar, quick, and does not have to be done in sterile conditions. However, this can be difficult due to the small size of a neonate.
The smallest EZ-IO needle is 15mm long and for use in children 3-39kg. There is very limited data on locations other than proximal tibia for intraosseous placement in neonates.
A retrospective cross-sectional descriptive study of IO use in a single-center tertiary ED showed that EZ-IO success rate was lower in infants who weighed ≤ 8kg compared to infants who weighed more than 8kg (p-value = 0.005). There were significant differences in performance between manual and EZ-IO devices in children ≤ 8kg. [2]
Quick Tip
Because of this, Dr Gary Geis (one of our esteemed faculty members) has this tip for us-- insert the IO manually in these tiny babies!
Resuscitation of Neonatal Shock
There a certain things to keep in mind when resuscitating an ill neonate.
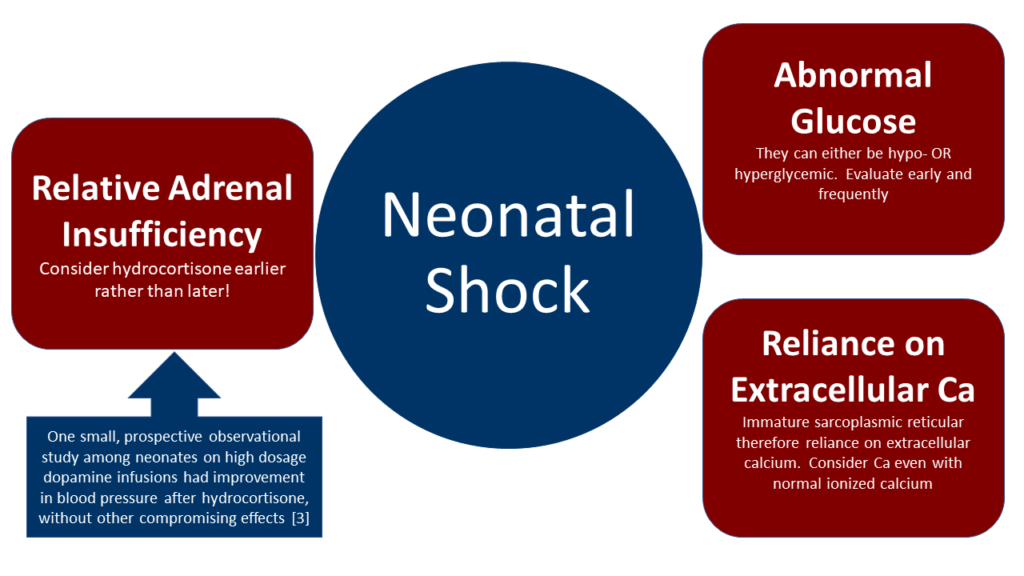
What about Pressors?
There is poor data to suggest superiority of specific vasoactive agents.
A randomized control trial comparing epinephrine and dopamine among 40 neonates in fluid-refractory shock showed no significant differences in reversal of shock, ability to maintain hemodynamic stability, or all-cause mortality. Although, neonates < 31 weeks treated with epinephrine had better outcomes. [4]

1. Neonates have can unique etiologies for shock, especially cardiac. If it’s not on your mind, you’ll miss it.
2. IV access may be a problem. Consider manual intraosseous or central access in critically ill neonates.
3. Management of neonatal septic shock should account for unique aspects of neonatal physiology.
References
- Anderson, J., et al., Umbilical Vascular Catheterization. New England Journal of Medicine, 2008. 359(15): p. e18. https://www.nejm.org/doi/full/10.1056/NEJMvcm0800666
- Pifko, E. L., Price, A. , Busch, C. , Smith, C. , Jiang, Y. , Dobson, J. and Tuuri, R. Observational review of paediatric intraosseous needle placement in the paediatric emergency department. J Paediatr Child Health, 2018;54: 546-550. doi:10.1111/jpc.1377
- Noori S, Friedlich P, Wong P, Ebrahimi M, Siassi B, Seri I. Hemodynamic changes after low-dosage hydrocortisone administration in vasopressor-treated preterm and term neonates. Pediatrics. 2006 Oct;118(4):1456-66
- Baske K, Saini SS, Dutta S, Sundaram V. Epinephrine versus dopamine in neonatal septic shock: a double-blind randomized controlled trial. Eur J Pediatr. 2018 Sep;177(9):1335-1342

Ronine Zamor is a 3rd year pediatric emergency medicine fellow at CCHMC, with research interests in health disparities and global health. She loves traveling to see new places, and anything that has to do with Haiti (including Haitian food, people, music!).




