Could it be... The Heart?
A newborn presents to your emergency department. The baby is 2 weeks old, and parents are bringing him in because he has not fed well for the past 24 hours, and does not seem to be acting like himself. You take one look at this baby and see a lethargic, ill appearing baby. Sepsis should always be considered for these babies, but another diagnosis that should be high on your differential is congenital heart disease.
A Framework for Newborn Congenital Heart Disease
Rather than attempting to identify the specific heart lesion present, many of these babies can fall into three categories that can then guide your treatment plan.

Your plan for treatment in the ED can be guided based on which of these categories your patient presents in based on the pathophysiology of their presentation.
Key to understanding these three categories is that the Gray Baby presents due to an obstruction to systemic circulation, while the Blue and Pink Baby present due to issues with pulmonary circulation.
Image edited from this free to use source.
The Blue Baby
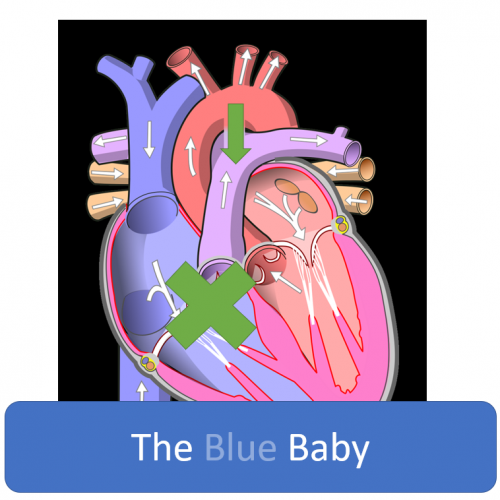
The blue baby presents due to lesions that obstruct right sided outflow obstruction, therefore decreases pulmonary blood flow. These babies present cyanotic, usually within the first 2 weeks of life. The cyanosis will be central– involving the mucous membranes, lips, tongue. Tachypnea, without other evidence of respiratory infection such as nasal congestion, wheeze, rhonchi, should raise your suspicion for CHD. A murmur could be present, but a lack of a murmur does not rule out CHD.
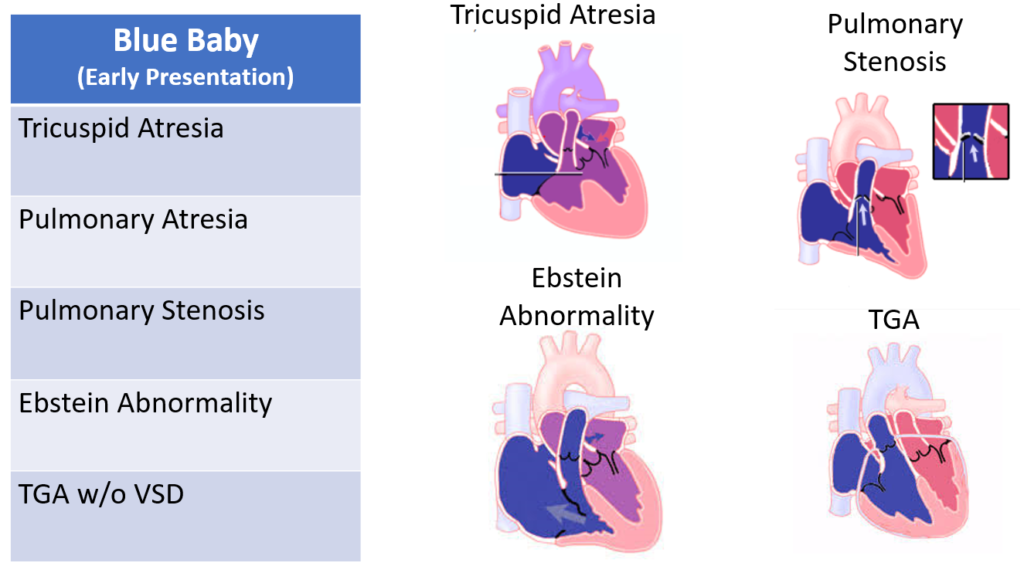
When these babies present blue in the ED, their PDA, which has sustained their pulmonary blood flow up until this point, is closing. These babies need an infusion of prostaglandins to maintain patency of their PDA until corrective cardiac surgery.
The Pink Baby
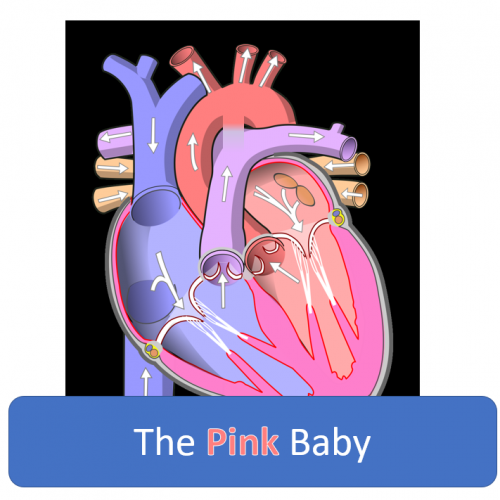
The pink baby presents due to too much pulmonary blood flow, which as the pulmonary vascular resistance falls throughout the first few months of life, leads to heart failure symptoms. Therefore, these babies usually present at ages 1-6 months. They often present with a history of poor feeding, including sweating or respiratory distress while attempting to feed, and poor weight gain. Exam findings may include tachypnea, crackles on auscultation, hepatosplenomegaly, or a murmur.
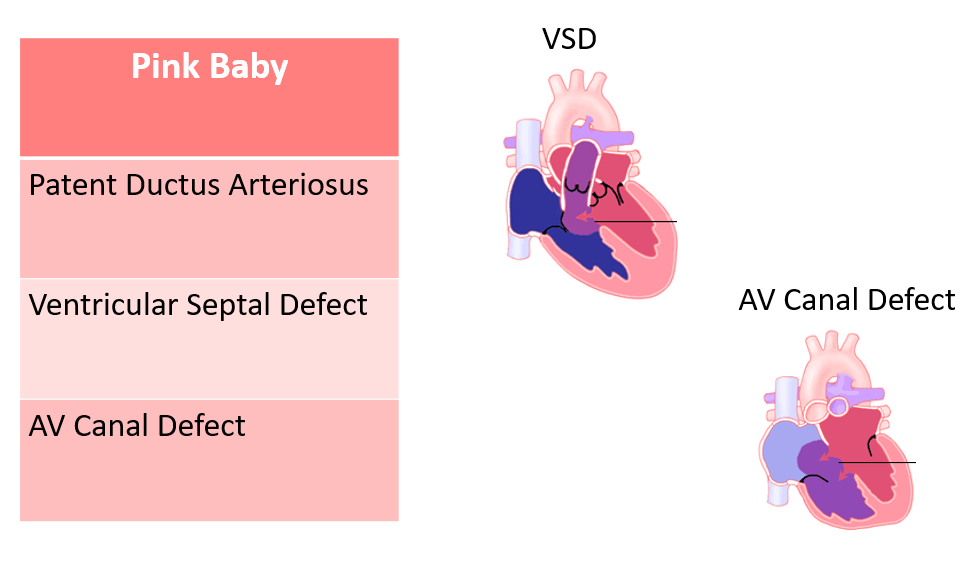
These babies become symptomatic and present to the ED with signs of heart failure. They have too much pulmonary blood flow, and too little systemic blood flow. They should not receive prostaglandins, and instead their heart failure symptoms should be managed while preparing them for pediatric cardiologist evaluation.
The Gray Baby
Similar to the blue baby, the gray baby presents early– usually within the first 2 weeks of life. They present grey due to a left sided obstructive lesion which is preventing systemic blood flow, therefore causing circulatory collapse. They are hypotensive with tachypnea, and can have a brachial-femoral pulse delay, systolic blood pressure differential greater than 10mmHg, and a positive pre/post ductal saturation screen. See Part 2 of this post for more information on these exam findings!
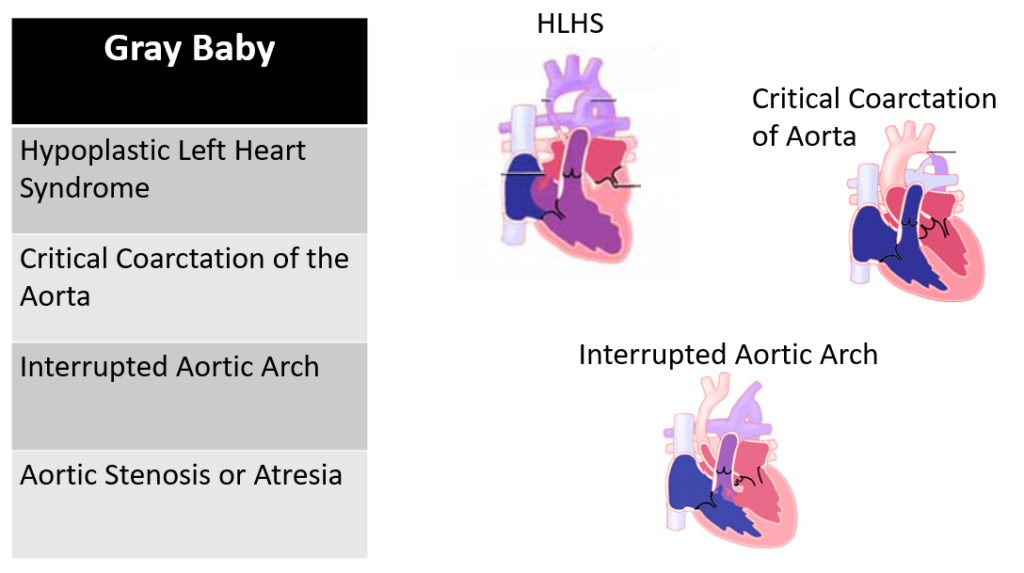
These babies can present with circulatory failure, therefore they need increased systemic flow across their PDA until definitive cardiac surgery can be performed. These babies need prostaglandin infusion on presentation to the ED.
Images of each of these congenital heart defects come from Cincinnati Children’s Heart Encyclopedia, which also has a mobile app version. This is a great resource to find more information about these specific heart lesions.
To read more about the presentation of newborn congenital heart disease, see this paper by Strobel et al, which is an awesome summary and was the basis of this blog post.
References
Strobel, A.M. & Lu, L.N. (2015). The critically ill infant with congenital heart disease. Emergency Medicine Clinics, 33(3), 501-518.
Heart Encyclopedia. Cincinnati Children’s Hospital Medical Center Website. https://www.cincinnatichildrens.org/patients/child/encyclopedia. Accessed April 14, 2014.

Katie Edmunds is a current Pediatric Emergency Medicine Fellow interested in creating PEM 4 all those who are given the responsibility of treating the sickest babies wherever they may be.



